Stoma Prolapse: Symptoms, Causes, and How To Fix

Stoma prolapse, a condition where the stoma elongates and protrudes more than intended from the abdominal wall, often raises many questions and concerns, particularly among individuals navigating the complexities of stoma management. This occurrence, while not uncommon, can be both physically and emotionally taxing, necessitating a nuanced approach to management and care.
In exploring the multifaceted aspects of stoma prolapse, from its initial identification to the myriad treatment options, considering the personal and emotional dimensions it encompasses is pivotal.
A prolapsed stoma can present challenges such as appliance fitting, maintaining a secure seal with the stoma bag, and managing potential skin complications, all crucial for preventing leakage and skin irritation.
Moreover, the emotional and psychological aspects, including feelings of anxiety, self-consciousness, or fear, should be acknowledged and addressed, ensuring comprehensive care that encompasses mental well-being. Engaging with a stoma care nurse or a stoma nurse for advice, local treatment, and support and exploring various stoma care strategies can be necessary in effectively managing a stoma prolapse.
Join us as we unravel the layers, providing a guiding light through the complexities of stoma and offering a beacon of knowledge and understanding in the often uncharted waters of managing stoma prolapse.
What is stomal prolapse?
Stomal prolapse, a condition where the stoma extends abnormally from the skin’s surface, presents a unique set of challenges and considerations in stoma management.
This condition, which can manifest as a minor to significant protrusion of the stoma, is not typically associated with pain but does introduce hurdles in maintaining a secure seal loop stomas and effectively fitting stoma appliances, which is crucial to prevent leakage and subsequent skin irritation.
While stomal prolapse may evoke concern due to its altered appearance, stoma functions, and the potential management issues it introduces, it’s imperative to underscore that with appropriate medical guidance, perhaps from a stoma care nurse, and employing specialized stoma care strategies, this condition can be effectively managed.
Whether navigating through the nuances of ostomy surgery, exploring the realms of stoma prolapses, or seeking to understand the intricacies of managing a loop colostomy, the journey through understanding and managing stomal prolapse necessitates a blend of deep knowledge, practical strategies, and an empathetic approach to ensure optimal quality of life and effective stoma management.
What are the symptoms of prolapsed stoma?
This condition presents visible alterations, such as a stoma in the protruding bowel that appears longer and more protruded, but also brings forth potential complications that warrant keen attention and adept care.
Visible Alterations and Physical Discomfort
A prolapsed stoma, notably characterized by swelling, a change in appearance, and sometimes extending significantly from its usual position, can introduce varying degrees of discomfort, especially when engaging in activities that exert pressure on the abdominal muscles. This is particularly true for individuals with weak belly muscles, where the extra pressure may exacerbate the prolapse.
Challenges in Appliance Management
The altered physical state of a prolapsed stoma can usher in challenges related to stoma appliance management. The misfit of stoma appliances, such as bags or pouches, can lead to leakages, posing not only practical challenges but also the risk of skin irritation and infection around the stoma site due to prolonged exposure to waste.
Here, employing a support garment might be a viable option to ensure secure appliance placement and manage the prolapse effectively.
Skin Complications
Skin complications, especially involving the peristomal skin, often accompany a prolapsed stoma, particularly in severe patients when appliance mismanagement leads to leakage.
In severe instances, persistent exposure to waste may necessitate surgical intervention to address infections and alter stoma care practices, ensuring the skin is adequately protected and managed.
Navigational Challenges in Daily Activities
Daily activities, especially those involving bending, stretching, or engaging the belly muscles, may require additional caution and modified techniques for individuals experiencing a prolapsed stoma.
This prevents exacerbating the prolapse or inducing discomfort, ensuring that activities are navigated with minimal risk to the stoma.
Emotional and Psychological Implications
Addressing the emotional and psychological terrain that may need to be traversed when dealing with a prolapsed stoma is pivotal. The altered physical appearance and potential for leakage may instill anxiety or self-consciousness in various settings.
Thus, ensuring emotional support, alongside physical management strategies, becomes integral in holistically addressing the implications of a prolapsed stoma.
In conclusion, managing a prolapsed stoma, especially in cases where surgical repair or other interventions like applying a cold compress or employing a mesh strip technique may be considered, necessitates a blend of adept knowledge, practical strategies, and emotional support.
Whether managing a colostomy prolapse, exploring surgical procedures, or understanding the implications of weight gain on your stoma size and stability, the journey through understanding and managing a prolapsed stoma is enriched by shared experiences, medical advancements, and a compassionate approach to care.
What causes a stoma to prolapse?
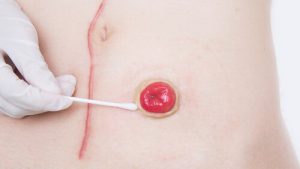
A prolapsed stoma, can manifest due to various factors, each contributing to the alteration of the stoma’s physical state and, subsequently, its management.
Physical Strain and Exertion
One of the prominent causes of stoma prolapse revolves around physical strain and exertion of abdominal muscle. Activities or situations that increase abdominal pressure, such as coughing, lifting heavy objects, or straining the abdomen during bowel movements, can exert pressure on the stoma, potentially leading to its prolapse.
The increased intra-abdominal pressure pushes against the stoma, causing it to protrude more than its usual state, thereby leading to a prolapse.
Surgical Techniques and Post-Operative Management
The techniques employed during the first surgical procedure, the creation of the stoma, and the post-operative management can also influence the likelihood of a prolapse—factors such as the placement and construction of the stoma and managing abdominal pressure post-surgery play pivotal roles.
Ensuring meticulous surgical technique and optimal post-operative care is crucial in mitigating the risk of developing a prolapsed stoma.
Anatomical and Physiological Factors
Anatomical and physiological factors can also contribute to stoma prolapse, including muscle weakness in the muscles supporting the abdominal wall or conditions predisposing an individual to increased abdominal pressure.
For instance, obesity, associated with elevated intra-abdominal pressure, may increase the risk of experiencing a stoma prolapse. Similarly, pre-existing conditions that weaken the abdominal muscles might also predispose an individual to stoma prolapse.
Chronic Conditions and Ongoing Strain
Chronic conditions, such as chronic obstructive pulmonary disease (COPD), which involve persistent coughing or conditions that lead to regular straining during bowel movements, can perpetually exert pressure on the stoma, increasing the risk of prolapse.
Managing these chronic conditions and mitigating their impact on stoma stability becomes paramount in these contexts.
Aging and Muscular Atrophy
Aging and the associated muscular atrophy or weakening can also contribute to stoma prolapse. As the colon and body age, the muscles around the stoma may weaken, reducing the support and stability of the stoma and potentially leading to a prolapse, especially when coupled with other risk factors.
Method to fix the stoma to the abdominal wall
The method to fix the stoma to the abdominal wall is not merely a surgical endeavor but a holistic approach to end stomas that encompasses various stages and strategies, each tailored to enhance the stoma’s stability and functionality while ensuring the individual’s well-being.
Surgical Precision: Stoma Creation and Fixation
- Strategic Planning: The initial phase involves strategic planning, where the surgical team meticulously determines the optimal location for the stoma, considering factors such as the patient’s anatomy, lifestyle, and ease of management.
- Surgical Technique: Employing a surgical technique that ensures the stoma is adequately mobilized and fixed securely to the abdominal wall is paramount. This may involve suturing the stoma to the peritoneum and abdominal wall, ensuring stability and minimizing the risk of complications such as prolapse or retraction.
- Post-Operative Assessment: A thorough post-operative assessment to ensure the stoma is securely fixed and functioning optimally is crucial, involving regular checks for signs of complications and ensuring the stoma is adhering well to the abdominal wall.
Post-Operative Care: Ensuring Ongoing Stability
- Stoma Education: Educating the patient and caregivers about managing the stoma, recognizing signs of complications, and ensuring ongoing stability is crucial. This involves practical demonstrations and providing resources to empower individuals in their stoma care journey.
- Routine Checks: Implementing a schedule for routine checks to assess the stoma’s stability, adherence to the abdominal wall, and overall health, ensuring any issues are promptly identified and addressed.
- Support and Adaptation: Providing ongoing support and adaptations, such as stoma belts or supports, to ensure the stoma remains securely fixed, especially during physical activities, is vital.
Long-Term Management: Navigating Through Daily Life
- Lifestyle Adaptations: Engaging in lifestyle adaptations that minimize strain on the stoma, such as avoiding heavy lifting and ensuring gentle and effective management of the stoma, is pivotal.
- Regular Assessments: Ensuring regular assessments with healthcare professionals to monitor the stoma’s stability and adherence to the abdominal wall, adapting strategies as needed.
- Community and Support: Engaging with the stoma care community and healthcare professionals to navigate through challenges, share experiences, and gain insights into managing and ensuring the ongoing stability of the stoma.
Stoma prolapse handmade repair
Addressing a stoma prolapse, especially considering a handmade or at-home repair, demands a delicate balance of practicality, safety, and adherence to medical advice. It’s crucial to note that a healthcare professional should conduct any significant alterations to a stoma to prevent complications.
Is a prolapsed stoma dangerous?
A prolapsed stoma, characterized by an elongation of the stoma beyond its usual length, can be a source of concern for individuals living with an ostomy, intertwining both physical and emotional dimensions of their ostomy journey.
- Physical Implications: While a prolapsed stoma is generally not considered an immediate danger, it does bring forth various physical implications that warrant attention. These include the potential for increased irritation, difficulty in appliance management, and susceptibility to trauma or injury due to its protrusion.
- Risk of Complications: There are instances where a prolapsed stoma may present more significant risks, particularly if it becomes incarcerated or strangulated, restricting blood flow and potentially leading to tissue death, which is a medical emergency.
- Quality of Life Impact: Beyond the physical, a prolapsed stoma can impact an individual’s quality of life, affecting their confidence, social interactions, and daily activities due to concerns about appliance security, leakage, and appearance.
- Management and Care: Effective management and care of a prolapsed stoma, involving appropriate appliance selection, gentle handling, and regular monitoring, are pivotal in minimizing risks and ensuring optimal stoma function.
- Medical Oversight: Regular check-ups and open communication with healthcare professionals ensure that any changes or concerns regarding the stoma, particularly in prolapse, are addressed promptly and appropriately.
- Emotional and Psychological Aspect: The emotional and psychological aspects of dealing with a prolapsed stoma, including anxiety, self-consciousness, or fear, should be acknowledged and addressed, ensuring comprehensive care that encompasses mental well-being.
What do I do if my stoma prolapses?

A prolapsed stoma necessitates a blend of immediate care and professional consultation.
- Immediate Response: Initially, it’s imperative to remain calm and assess the stoma, ensuring no immediate risk, such as strangulation or notable discoloration that may indicate a lack of blood flow.
- Support and Protection: A stoma guard or a supportive belt can temporarily support and protect the prolapsed stoma from further trauma or damage.
- Ostomy Care: Ensure that the ostomy appliance fits well around the prolapsed stoma, potentially necessitating a change in the size or type of the ostomy appliance used.
- Professional Consultation: Engage promptly with your healthcare provider or stoma nurse, detailing the occurrence and any accompanying symptoms or changes.
- Monitoring: Keep a vigilant eye on the stoma, noting any alterations in color, size, or output, and communicate these to your healthcare professional.
- Adaptation of Care Techniques: Be prepared to adapt your stoma care routine, incorporating any advised changes or adjustments to manage the prolapsed stoma effectively.
- Emotional and Psychological Support: Engage with support groups, therapists, or counselors to navigate through the emotional and psychological aspects that may accompany dealing with a stoma prolapse.
Conclusion
Stoma care demands a harmonious blend of adept knowledge and compassionate understanding, especially when confronted with a prolapse. As we encapsulate our exploration, it’s pivotal to underscore that while a stoma prolapse can introduce new challenges and necessitate alterations in care strategies, it is through the amalgamation of proficient medical oversight, effective management techniques, and nurturing emotional support that individuals can continue to lead fulfilling lives.
The tapestry of experiences, challenges, and triumphs in managing a stoma prolapse is rich and varied, and as we forge ahead, the collective wisdom, shared stories, and medical advancements continue to illuminate the path toward enhanced care, understanding, and support for every individual embarking on this journey.
References
Stoma Prolapse: A Comprehensive Review of the Literature
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9650348/
Managing your stoma prolapse
https://www.cuh.nhs.uk/patient-information/managing-your-stoma-prolapse/
What to Know About Colostomy Prolapse
https://www.healthline.com/health/colostomy-prolapse
Prolapsed Stoma
Prolapsed Stoma
https://www.med.umich.edu/1libr/Surgery/GenSurgery/ProlapsedStoma.pdf

